Election 2023: How Parties Score on Issues of Reproductive Justice
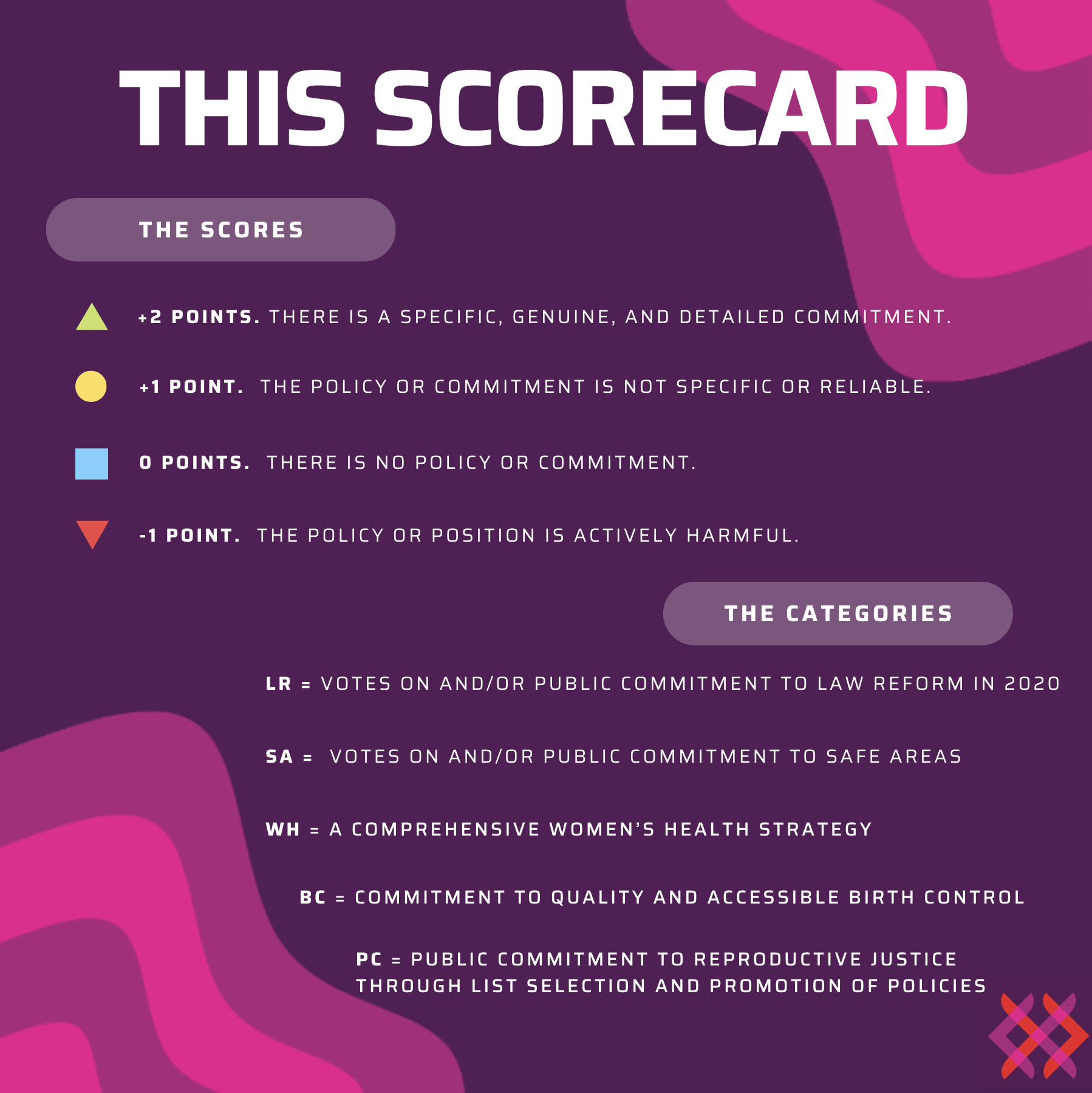
On 14 October 2023, Aotearoa New Zealand will go to the polls to vote on who they want to represent them in Parliament. ALRANZ has been consistent that reproductive rights are on the ballot this election. From implementing safe areas, to funding contraception, to the general global rollback of women’s rights, voters should be confident they are voting for a party that can be trusted with these important issues. ALRANZ has gathered data on five different metrics for these scorecards from publicly available sources in order to make an assessment on which parties will be good for reproductive rights, and which parties will stagnate (or even reverse) progress.
First, Act (well, David Seymour) voted in favour of abortion law reform in 2020 and has been a long-standing proponent of the idea the state should not interfere in private medical decisions. While ultimately voting yes to safe areas in 2022, David Seymour was the reason the provision was removed from law reform in 2020. Furthermore, both David Seymour and Deputy Leader Brooke van Velden have made public comments expressing concerns about safe areas and freedom of speech. (You can read ALRANZ’s position on those concerns here.) ALRANZ is therefore unconvinced ACT would actually implement safe areas if they got into power. There is no mention of anything related to women’s health, rights, or reproductive justice in the rest of ACT’s material for this election.
The Green Party have been consistent and dedicated allies to the reproductive justice movement. The entire caucus voted in favour of both law reform and safe areas. The caucus has also been outspoken on issues of reproductive justice globally, issuing statements on things like the overturn of Roe v Wade in the United States. While not specifically mentioning future issues to do with reproductive rights, the Green Party manifesto mentions involvement in 0800 DECIDE, and notes the Green Party wants to finalise and resource the women’s health strategy. The women’s health strategy includes issues of access to contraception. ALRANZ is confident on the Green Party’s commitment to reproductive justice.
80 per cent of the Labour Party caucus voted in favour of abortion law reform in 2020. The top 5 on Labour’s current list (Chris Hipkins, Kelvin Davis, Carmel Sepuloni, Grant Roberston and Megan Woods) all voted in favour. 95 per cent of the Labour caucus voted in favour of safe areas, all MPs in the top 20 on Labour’s current list. This commitment on paper has become a reality: 11 providers have had safe areas implemented under a Labour-led government and Labour introduced the 0800 DECIDE helpline. The information about Labour’s position on issues of reproductive justice are easy to find in their “women’s health manifesto”, which shows these issues are a priority for them. Labour have comprehensive policies on maternal health, birth injuries, cervical cancer, breast cancer, endometriosis treatment, funding period products in school, removing prescription fees for access to contraception and increasing Pharmac funding to explore birth control options.
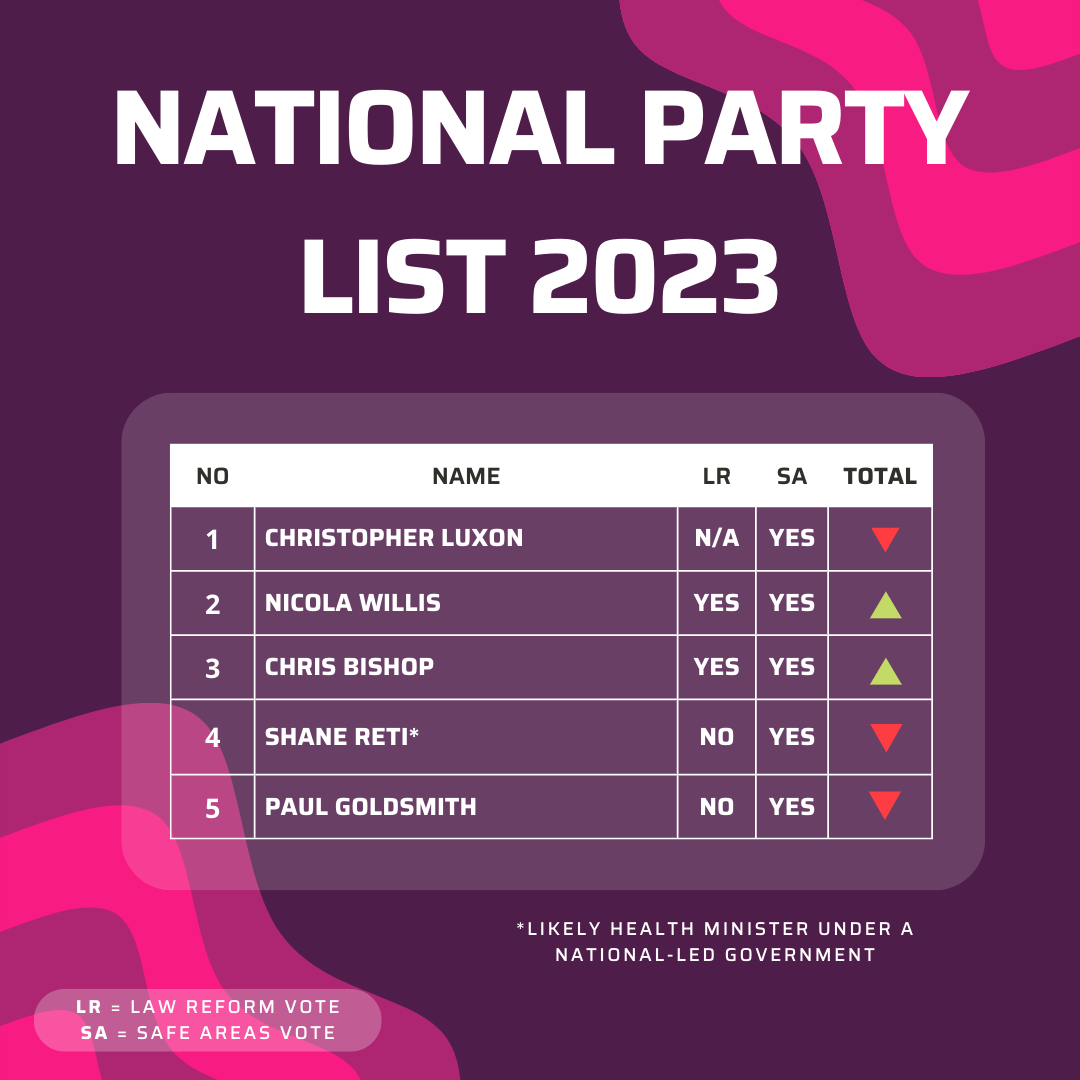
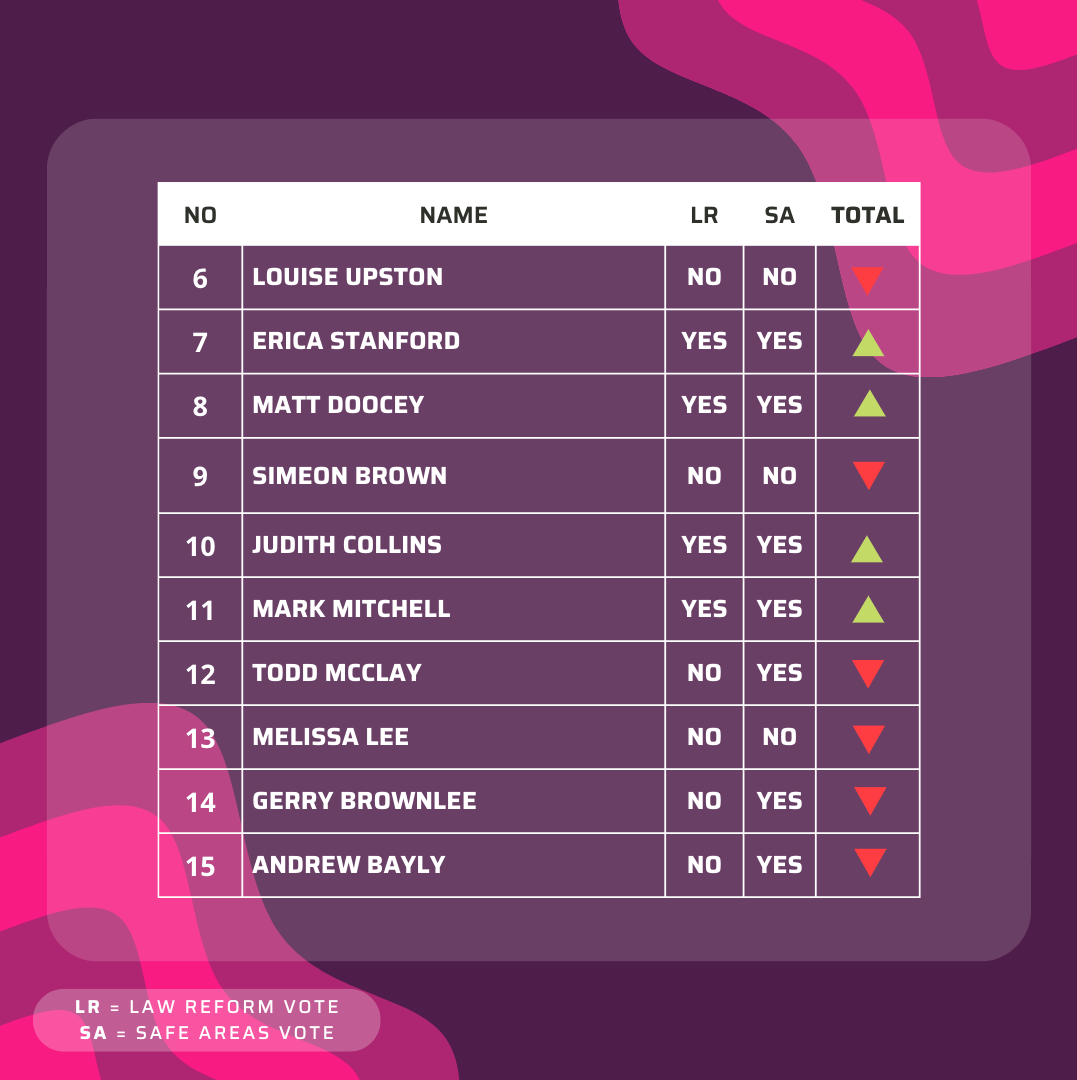
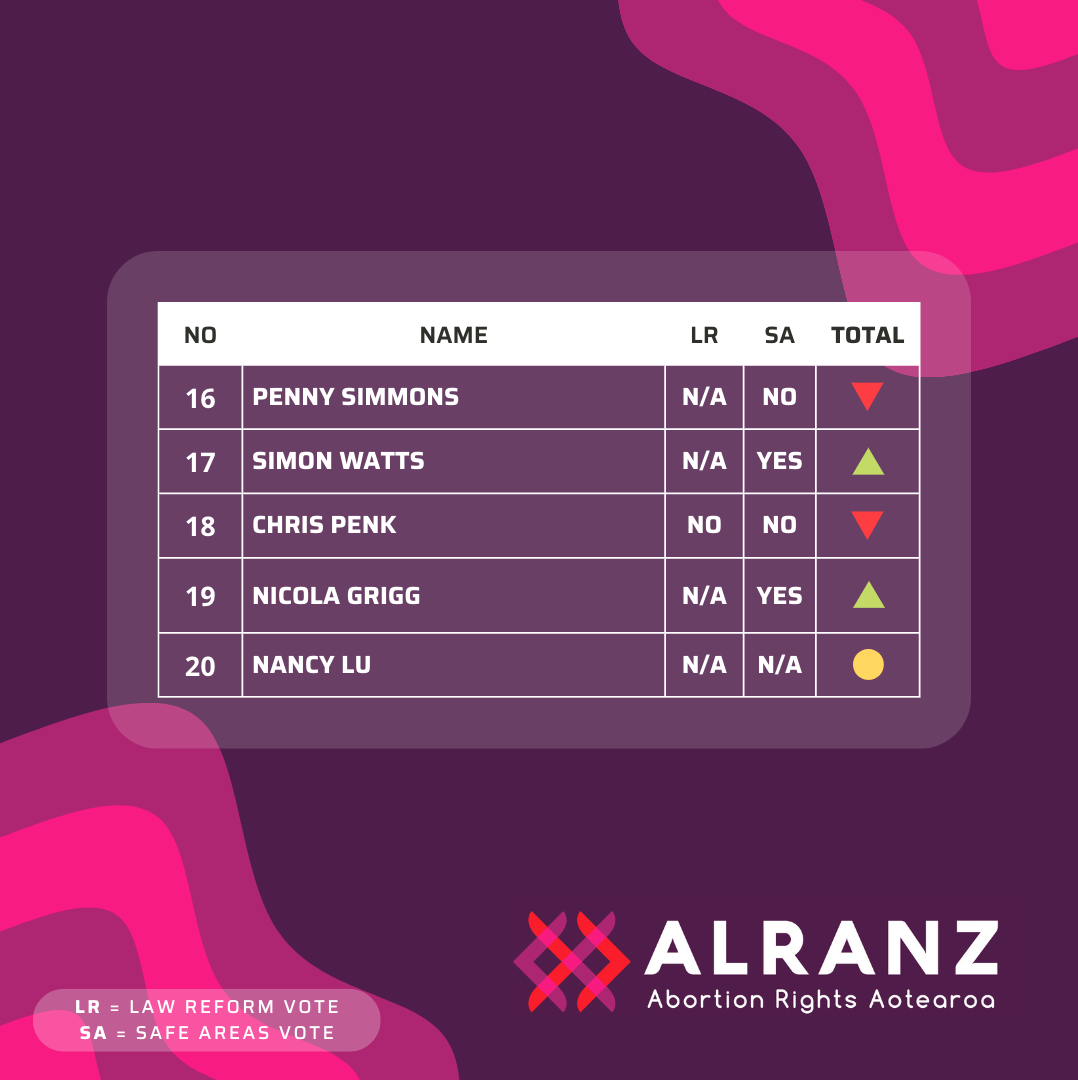
The National Party have a chequered history with reproductive rights. Just 35 per cent of caucus voted in favour of law reform in 2020. In the National Party’s current list, number 4 and 5 (Shane Reti and Paul Goldsmith) both voted no. While all of the top 5 (along with 73 per cent of the caucus) voted yes to safe areas in 2022, ALRANZ is sceptical of National’s willingness to preserve or implement safe areas given Reti and Goldsmith would be the Ministers of Health and Justice (respectively) under a National-led government. National do not have a general women’s health policy, but have committed to expanding free breast cancer screenings. National wish to re-introduce prescription fees for contraceptive drugs, although Deputy Leader Nicola Willis did hint National were “looking into” long acting reversal contraceptives (LARCs). ALRANZ is concerned about a National led government in large part due to the anti-choice beliefs of leader Christopher Luxon. This is reflected in his caucus: 50 per cent of National’s top 20 got a downwards vote from ALRANZ in our previous scorecard.
New Zealand First were the only party to get a score in the negative numbers, in large part due to their complete silence on all issues of women’s rights and reproductive justice. Publicly, what we know is that just 22 per cent of the New Zealand First caucus (two MPs) voted for law reform in 2020. Winston Peters, Shane Jones and Mark Patterson all voted no (numbers 1, 2 and 5 on the New Zealand First list). Both Te Pāti Māori MPs voted yes on safe areas in 2022, but otherwise have shown little public engagement with issues of reproductive rights. Some of this may be due to the health policy on their website being a dead link. Finally, TOP’s website contained easy-to-find policies, including one on fully funding contraception (including LARCs), fully funding antenatal ultrasounds and prioritising women’s health. Despite not being in Parliament during law reform or safe areas, TOP have been dedicated and consistent advocates of reproductive justice (and great friends to ALRANZ).
While who to vote for is a choice for each individual voter, ALRANZ implores everyone to decide what level of risk you comfortable with this election. Because we only need to look overseas to see the devastating effects electing people who are not pro-choice can have.
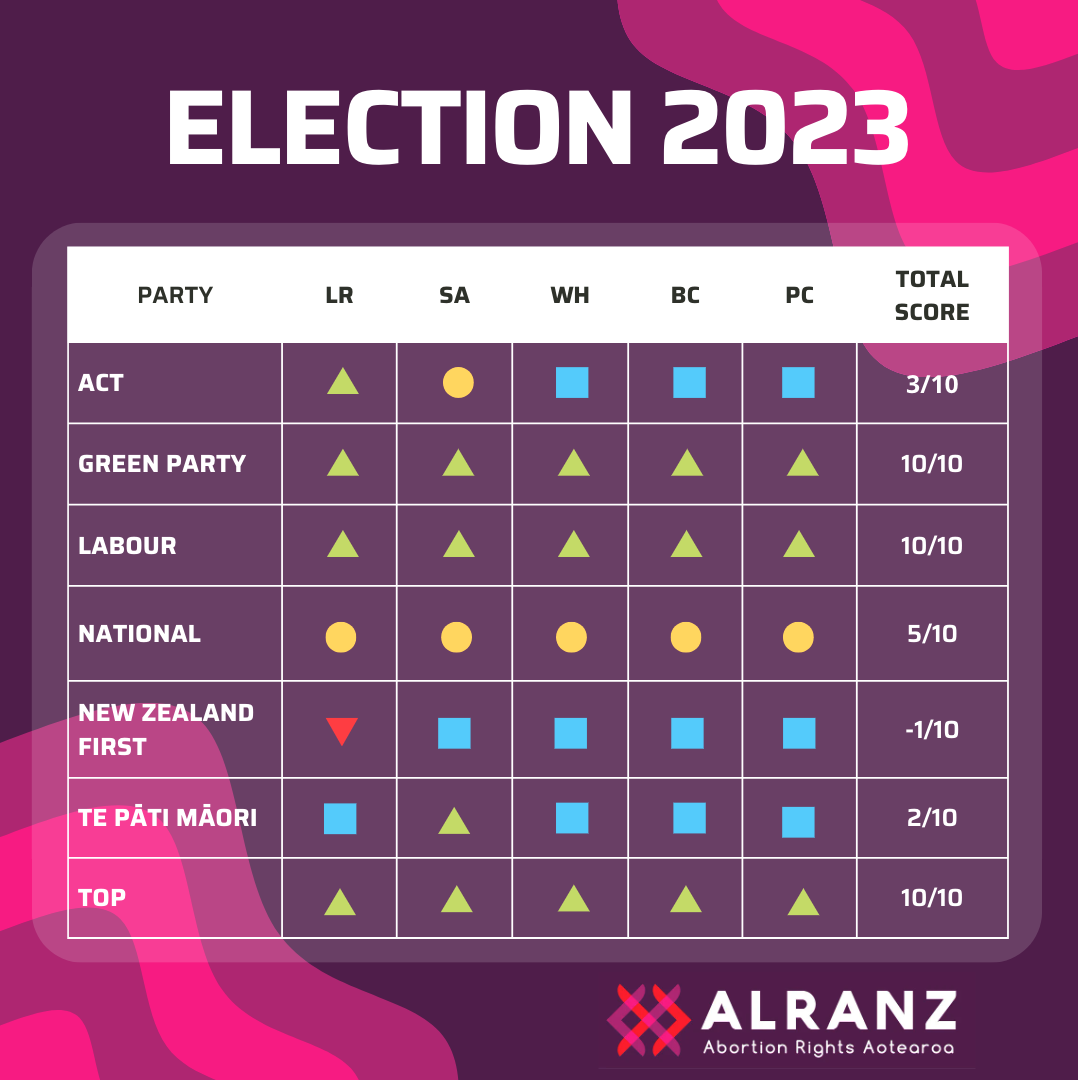

If you believe any information on this scorecard is not an accurate reflection of a party’s policy or position, please contact ALRANZ here. Please include in your message a reference to publicly available information that contradicts what ALRANZ has said.