Cross-posted from The Hand Mirror.
By Alison McCulloch
Back in the 1960s, when the Pill became available in Aotearoa New Zealand, the New Zealand Branch of the British Medical Association (the precursor to today’s NZMA) decided it would be unethical for doctors to let unmarried women get their hands on it. Doing so, it was argued, would be akin to doctors giving extra-marital relationships a stamp of approval, and the NZMA wasn’t about to do that.
If you thought doctors keeping us from the Pill for our own good was a thing of the past, think again. Sure, it’s no longer under the guise of protecting our moral purity – (most) doctors have (mostly) given up on that argument. Now, it’s all about protecting our health.
As recently as 1996, both the Royal College of General Practitioners and the NZMA opposed the reclassification of the Emergency Contraceptive Pill. “We have concerns that in a pharmacy the patient may be disadvantaged from receiving the greater advice that would occur in a general practice consultation,” the college’s chairman, Professor Gregor Coster, was quoted as saying in an article in the British Medical Journal.
Fast forward to 2016, and a new front in this seemingly endless struggle is focused on efforts to get the Pill, aka oral contraception, liberated from doctors’ prescription pads and made available over the counter. The most recent round began in 2014, when Pharmacybrands Ltd (now Green Cross Health, which represents 300 community pharmacies and has an equity interest in 80) and Pharma Projects Ltd, now Natalie Gauld Ltd., made an application to Medsafe’s Medicines Classifications Committee to reclassify the Pill so it could be sold in pharmacies without prescription, though only by specially trained pharmacists, following the model that’s now used for the Emergency Contraceptive Pill.
That application was turned down in the face of stiff opposition from general practitioners and the NZMA: the latter said they didn’t think prescription only access was a barrier to the Pill and wanted to make sure doctors continued to provide “the advice and counselling about its use and about sexual health in general”, while the College of GPs, apparently felt “as if they are being excluded from an important part of primary health care”. (Never mind that the actual users of this “important part of primary health care” were – and continue to be – excluded.)
On the plus side, the New Zealand Committee of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists (is that a long enough title for you?) backed the reclassification saying it was “strongly in support of any responsible development designed to improve access to quality contraceptive advice and service”.
Not to be discouraged by the initial setback at Medsafe, the applicants tried again early in 2015, and were – again – rejected. This time, however, they lodged an objection to the decision and at the same time proposed an alternative to the Emergency Contraceptive Pill model, whereby only women who have previously had oral contraceptives prescribed by a doctor could access the medication without a script at a pharmacy.
It was all looking pretty rosy when the committee went along with the “previous prescription” model and said yes. But wait, not so fast. Perhaps still feeling “excluded”, the Royal New Zealand College of GPs lodged their own objection earlier this year, arguing that there had been no public consultation on Green Cross’s “been previously prescribed the pill” idea. The College put out a media release explaining what they’d done, and re-stating their firm opposition to any loosening of doctor control over oral contraceptives: “Our members strongly opposed the original application to reclassify the oral contraceptive pill on the grounds that while it is a safe and effective contraceptive for the majority of women, for some women it is not, and alternative contraception methods need to be prescribed.”
It’s worth noting at this point that GPs are actually pretty well represented on Medsafe’s Classifications Committee, which leads inquiring minds to wonder whether or not they might have a conflict of interest when it comes to the prospect of losing repeat Pill-prescribing business. According to minutes from the April 2014 and May 2015 meetings, however, none of the Committee members, reported themselves for having any such conflicts.
And of course, on the applicant side of the equation, having more medicines available from pharmacies is certainly better for their bottom line as well. Indeed, there’s a bit of a turf war going on between doctors and pharmacists as a recent New Zealand Doctor article made clear. Titled “General practice get ready – pharmacy is on the rise”, the article points out that that the government is more than eager to see pharmacists take on more of the work GPs have traditionally done. Though the article doesn’t say so, it’s hard to avoid the conclusion that this, too, has something to do with the bottom line.
HOW IT MIGHT WORK
Dr. Natalie Gauld, one of the applicants seeking reclassification, is a pharmacist and sat on the Medsafe Classifications Committee from 2004 to 2009. She told me therewere a few medicines she thought could be available without a prescription, including oral contraception, and when she left the committee, she started working with Green Cross on trying to get them reclassified.
While she doesn’t want to talk about Medsafe’s decision-making while it’s still going on, she did explain how accessing the Pill over-the-counter might work for New Zealand women.
“A model increasingly used in New Zealand is pharmacists being specially trained, and using a questionnaire – a screening tool. What it means is that it’s not a two-minute ‘go and ask for something and leave’, but it would be a careful consultation. So even if somebody has got it from the doctor in the last three years, there’s still going to be a health professional responsibility to ensure that the woman fits the criteria that allows the pharmacist to supply it.
“So for the combined oral contraceptive, it would be things like a blood pressure check once a year, and … checking for things like migraines, and age and other risk factors to ensure that women at a higher risk of side effects that are important won’t be supplied through the pharmacist.”
HOW MUCH MIGHT IT COST?
Cost decisions are separate from decisions about reclassifying a medicine – Pharmac and DHBs usually sort out the funding, while Medsafe sorts out where and how medicines can be sold. In some areas, for example, the Emergency Contraceptive Pill is funded for young women when they get it without a prescription from the pharmacy, but not in all areas. So the DHBs sometimes choose to fund drugs through pharmacies differently in different areas.
If there isn’t any funding for the Pill at the pharmacy, which is the most likely outcome, the cost could be around $45 for a three-month supply. However, women could still access the Pill through their doctor or Family Planning clinic, in which case the status quo would apply: the cost of the consultation (free for under-22s at Family Planning) plus the standard prescription fee of $5.
IS IT SAFE?
So what about these arguments GPs and the NZMA like to make that letting women decide for themselves whether or not to take the Pill is just too dangerous? There are rafts of studies looking at the risks and benefits of widening access to the Pill – and two great places to read about some of them are at the U.S.-based “OCs OTC” (Oral Contraceptives Over-The-Counter) and “Free the Pill”.
As Free the Pill points out, the risk of misuse or abuse is low “you can’t overdose on the pill”; the directions are simple “you just take one every day”; women are smart enough to use checklists to assess their own risks; not to mention that the Pill has health benefits in addition to the big one of preventing unplanned pregnancy: “It reduces pain and heavy bleeding with periods, helps prevent acne and anaemia, reduces the risk of certain cancers, and more. A study in the medical journal The Lancet showed that over the last 50 years the pill has prevented 200,000 cases of ovarian cancer and 100,000 deaths from the disease.”
Lots of other countries allow it, particularly in the Global South, with moves to expand access in the U.S. and U.K. (For the proper interactive version of this map, click here – or just click on the map.)
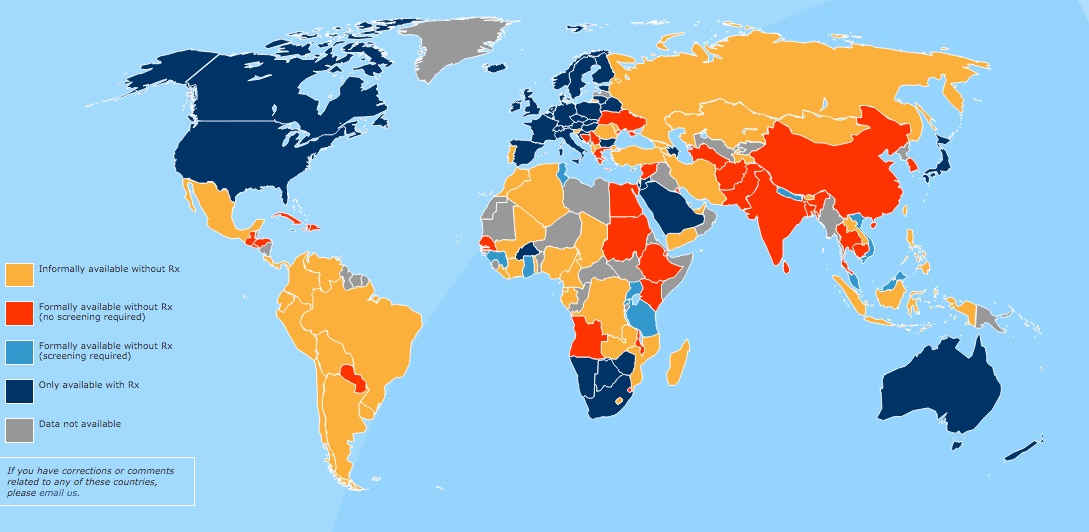
‘Global Oral Contraception Availability. From the OCs OTC (Oral Contraceptives Over the Counter) Working Group
In January of this year, a law allowing over the counter sales – though only through specially trained pharmacists and only for women aged 18 or over – came into effect in the U.S. state of Oregon, with California about to follow suit and Colorado, Washington and New Mexico thinking about it.
Oregon and California have faced the usual critics, plus some on the other side of the issue, who argue their laws don’t go far enough to improve access to contraception. Here at home, as ALRANZ pointed out in a perhaps prematurely positive media release, the “previously prescribed” model is only a start. We need better access – which includes affordability – to all forms of contraception, not just the Pill.
In the end, it’s hard to see how making this medication hard to get isn’t rooted in good old paternalism and moralism whereby doctors, churches and governments want to keep control over female sexuality. That, mixed with a little bit of self interest. Sometimes, it feels like the 1960s aren’t that long ago after all.
LINKS:
- Last year, the Abortion Law Reform Association (of which I’m a member) put in a submission supporting the reclassification, as did Dame Margaret Sparrow.
- If you want to have your say in the latest round, please do so by 5 April for the next meeting, and information on how to do so is here.
- Free the Pill and OCs-OTC
******************
CLICK HERE TO DONATE
TO HELP US CONTINUE OUR PRO-CHOICE WORK
